Prostate gland disease is one of the most common and insidious in men over 40 years old. At first, patients may not even know about the presence of a problem, but over time, the symptoms make themselves felt. If you do not consult a doctor in time, prostatitis becomes chronic and complications can arise. Depending on the severity, causes and nature of the course, different types of prostatitis are distinguished.
Types of prostatitis according to the shape of its course:
- acute;
- chronic;
- latency
What is prostatitis due to the appearance of:
- herpetic;
- bacterial;
- calculator;
- stagnant;
- infectious;
- purulent;
- chlamydial;
- fungi;
- gonorrhea;
- fijor.
Distribution
Faced with such an unpleasant disease of the genitourinary system as inflammation of the prostate gland, many men wonder why they have prostate.
Understanding the etiology of the disease helps in accurate diagnosis and effective prevention.
From the shape of the flow
According to the form of the course, prostatitis is divided into acute, chronic and latent, among which are distinguished catarrhal, follicular, parenchymal (purulent).
There are the following forms of the disease:
- With catarrhal prostate in the male body, there is a urination and disturbance disorder in the pubic region. This is the most common type of acute prostatitis.
- Follicular prostatitis is characterized by symptoms such as pain in the groin or anus, fever, and severe urinary disorders (dysuria). In a more advanced form, when the patient postpones the visit to the doctor, acute pain occurs during urination and urinary retention occurs.
- Parenchymal prostatitis - an abscess with purulent contents forms in the body of the prostate gland. In this case, fever occurs, sharp pains appear with a frequent desire to urinate. The temperature rises to 39-40 ° C, the act of defecation becomes almost impossible.
Acute prostatitis
Acute prostatitis is a condition in which there is inflammation of the prostate gland, which occurs in a short time and is characterized by various symptoms. Glandular edema occurs, provoked by the negative effects of pathogenic microflora. Disease-causing bacteria disrupt tissue integrity, causing permanent disturbances in the pelvic region, even at rest.
There are several prevalent ways for infection to enter the prostate gland:
- with inflammation of the rectum - lymphogenic route;
- after infectious diseases - hematogenous;
- directly through the urethra - canal.
Excessive accumulation of contents in the prostate gland creates excellent conditions for the growth of bacteria, which causes various complications:
- abscess;
- BPH;
- prostate cancer;
- loss of potency;
- infertility
The symptoms of prostatitis are so painful that the patient is obliged to urgently consult a doctor for help. If you do not do this in time, prostatitis will turn into a chronic form, which is much more difficult to cure. Antibiotic therapy in combination with drugs that strengthen the immune system effectively fights the disease.
Chronic prostatitis
Symptoms of chronic prostatitis are usually found against the background of congestion in the prostate gland, resulting from an untreated disease in an acute form. It usually occurs in men over 50 who have not sought help and are self-medicating. Many of them developed complications due to concomitant diseases. In addition, at this age, not everyone is quite sexually active, as a result of which the secretion thickens and gets stuck in the prostate, which leads to dysfunction. Interrupted relationships also provoke liquid stagnation. According to modern research, about 40% of men who experience symptoms of chronic prostatitis experience erection problems.
Chronic prostatitis, as a rule, has mild symptoms that appear only during an exacerbation. Patients notice dull pain in the groin area, which increases after physical exertion and at the end of the day. Often the pain radiates to the lower back, scrotum and perineum. Frequent urination is observed, especially at night, the electricity is intermittent, the discharge is crooked.
Sexual intercourse becomes shorter, incomplete erection is noticed, sometimes there is pain in the glans penis. Infertility is commonly found in men with chronic prostatitis; impotence at this stage of the disease practically does not exist. Sometimes there is a change in the color of the genitals, due to improper blood circulation, they become purple.
Each of the symptoms of prostatitis worsens if left untreated. The condition is similar to the manifestations in the acute course of the disease. Weakening of the immune system, stress, neglect of diet, bad habits - all this leads to deterioration and deterioration of the condition.
Often the chronic form leads to the appearance of symptoms of diseases such as cystitis, kidney disease and adenoma. The risk of urolithiasis and the formation of a malignant tumor increases. Often, the pathological process is almost asymptomatic and is detected quite by chance during laboratory tests associated with another disease.
Because of the occurrence
There are many reasons that provoke the development of prostatitis of infectious and non-infectious etiology, as well as predisposing factors. Due to the appearance, the following types of prostatitis are distinguished:
- bacterial;
- calculator;
- stagnant;
- infectious;
- purulent.
A sedentary lifestyle, frequent hypothermia, infrequent sexual activity, interrupted sexual intercourse, smoking, alcohol abuse, stressful situations - all these factors affect the stagnation of secretions in the vessels of the prostate gland and in the vessels oflocated next to it. Prostatitis is classified into several forms, depending on the reasons for its occurrence.
Bacterial prostatitis
Bacterial prostatitis is caused by bacteria that enter the prostate gland in different ways. It can be either a type of bacteria or a group of them. The disease can be caused by:
- fungi;
- gonococci;
- Koch stick;
- chlamydia;
- several types of bacteria at once.
The inflammatory process is most often associated with the penetration of bacteria into the prostate gland caused by sexually transmitted diseases. Rude sex with frequent change of partners and without the use of means of protection leads to diseases such as gonorrhea, chlamydia, fungal infections. In addition, the development of pathology is facilitated by a decline in immunity due to violation of the regime of work and rest. Bad habits, such as smoking, drinking alcohol, a sedentary lifestyle, etc. , Also reduce immunity.
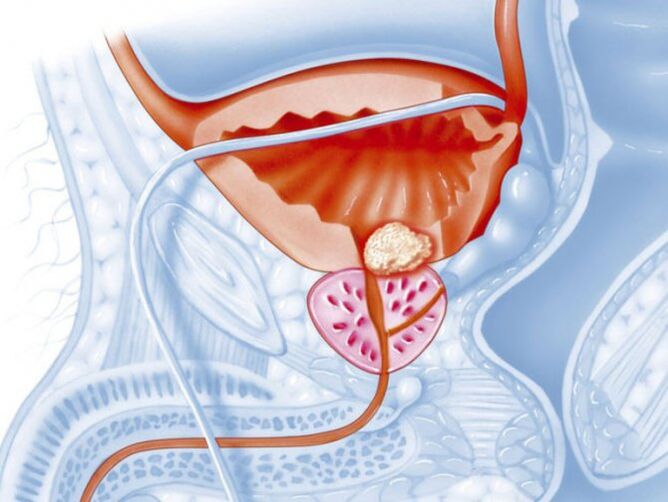
The most obvious symptoms that accompany bacterial-type prostatitis include burning, pain, and cloudy discharge when urinating. The smell of urine is unpleasant. General accompanying symptoms of intoxication are observed: dizziness, weakness, nausea, fever. Pain is noted during ejaculation, and sometimes blood is present. With chronic bacterial prostatitis, urination becomes more frequent, yellow or green discharge from the penis appears.
Calculated prostatitis
With calcified prostate, stones form in the ducts of the prostate gland. This form of the disease is very complex and is accompanied by severe pain. Conglomerates have different origins: phosphates, oxalates, with a predominance of calcium and protein.
There are two reasons for the appearance of stones in the ducts: stagnation of the contents of the gland and discharge of urine into the prostate.
Stagnation is associated with various factors that interfere with the normal flow of secreted fluid. Prolonged sexual abstinence, hyperplasia, the presence of a tumor that closes the ducts, and a sedentary lifestyle lead to stagnation of secretions and disruption of the vascular and lymphatic system.
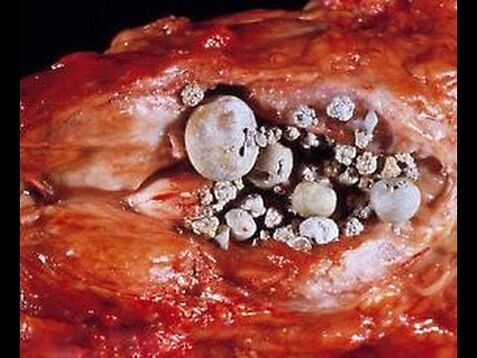
Urinary incontinence is caused by a sphincter dysfunction, which relaxes, and urine flows both outside and inside. The presence of stones and sand in the bladder contributes to the development of stones in the prostate ducts. They enter there with hunger, settle and continue their growth, eventually reducing output. Genital injuries and surgical interventions can lead to sphincter dysfunction.
At first, the calculating form of prostatitis is asymptomatic, as the stones grow, the symptoms appear and grow. There is soreness in the lower abdomen or scrotum, radiating to the buttocks and lower back. Pain at rest is not noticed and occurs only during physical exertion, the act of defecation and urination, as well as during sexual intercourse and while walking.
Large stones with sharp edges during their movement damage the canal, which leads not only to pain, but also to the release of blood in the urine and ejaculation. Stone sores can be easily infected, and then the calcified prostate will become infectious.
After about a month, with the prostate calculated, the work of the whole body breaks down, a person feels bad, experiences insomnia, increased fatigue and irritability.
In the advanced stages of calculating prostatitis, after a thorough diagnostic examination, a drug is prescribed and surgical treatment is performed to remove the conglomerates.
Congestive prostatitis
Stagnant onset of prostatitis occurs due to a delay in secretion into the prostate gland. Most often, such problems are observed in men with sedentary jobs, who are not involved in sports. As a result of hypodynamics, there is a violation of blood circulation in the pelvic organs, the prostate suffers from insufficient supply of oxygen and nutrients, stagnation and inflammation occur. If nothing is done, the disease becomes chronic and causes great concern.
Congestive prostatitis provokes irregular sex life or its complete absence. In this case, men should independently release the gland from the secretion, but do not overdo it, as regular masturbation can damage due to incomplete ejaculation. Many spouses have found for themselves such a way of preventing pregnancy as aborted relationships. It also leads to shedding and incomplete inflammation.
Sometimes hypothermia or varicose vein disease becomes a provocative factor. Abnormalities in the structure of the prostate gland can also cause stagnation. Regular overheating of the pelvic region and persistent constipation negatively affect the production of secretions. Depending on the factors that provoke the disease, several types of congestive prostatitis are distinguished.
- Venous prostates. Occurs in people with varicose veins of the lower extremities. In this disease, all the organs in the small pelvis are affected due to improper circulation.
- Congestive. It develops with partial emptying of the prostate gland. Gradual overload leads to stagnation.
- Chronicle. It develops when the wrong lifestyle has become a habit. If nothing is done to change the situation, the disease becomes chronic. Most often this happens to single men who suffer from overweight, already in adulthood, when the anamnesis is aggravated by concomitant diseases. At this stage, the prostate often enlarges, which is easy to determine during the examination.
- Infectious. It joins the already existing inflammation of the prostate when the infection enters the genitourinary system.
Manifested symptoms of prostatitis are caused by difficulty urinating, pain in the groin, tension during bowel movements and weakening of sexual activity. As a result of these symptoms, with stagnant types of prostatitis, poor health, irritability develops, the ability to work is reduced and sleep is disturbed.
Infectious prostates
Microorganisms that can provoke the appearance of signs of acute prostatitis include Escherichia coli, Staphylococcus aureus, Proteus, Eltirococcus, Klebsiella. There are bacteria that are constantly in the body, but in a dormant state they do not lead to inflammatory processes. When it penetrates through the urethra into the mucosa of the prostate gland, the process of development and reproduction of microorganisms begins, as a result of which inflammation develops. Indiscriminate and unprotected sex also allows harmful bacteria to enter the body.
Typical symptoms are pain in the scrotum, perineum, lower abdomen, spine, pain and burning sensation in the pelvis. Difficulty urinating, acute urinary retention occurs. In addition to the listed symptoms that accompany an infectious type of prostatitis, constipation, discharge from the urethra, hemospermia, and pain during ejaculation may occur.
It is a dangerous disease that, even in the earliest stages, is able to provoke an infection of a sexual partner, lead to general blood poisoning or to the development of pyelonephritis and cystitis.
Purulent prostates
Purulent prostatitis usually develops when a bacterial infection enters the prostate. The disease occurs in four stages.
- Catarrhal. It develops after suffering from acute viral respiratory infections, tonsillitis, influenza. Purulent contents are present in urine. There is a burning sensation when the bladder is empty. Patients notice a weakening of potency. The process that accompanies this type of prostatitis involves the superficial tissues of the prostate.
- Focal. The process extends to the glandular tissues. The canals swell, the flow is disturbed. The gland increases in size due to the accumulation of pus in it, which is excreted in the urine. Body temperature rises.
- Parenchymal. Connective tissue is involved in the process, the edema becomes even greater, the temperature can reach 40 ° C. The erupting pain in the anus spreads, the false desire to defecate is felt.
- Abscessive. The most insidious form of prostatitis. The temperature is severely disturbed, there is an abundant presence of pus and intolerable pain. This stage can be complicated by peritonitis and is fraught with death.
Purulent prostatitis can be complicated by symptoms and diseases such as paraproctitis, paracystitis, abscess, sepsis. Usually, these pathologies are treated surgically and involve the removal of purulent sacs.
Diagnosing
Diagnosing types of prostatitis is not particularly difficult and begins with collecting the anamnesis, which helps to more accurately understand the appearance of the disease. Then an examination of the colon is performed, during which the size of the gland is determined, the nature of the pain is determined, the presence of edema and seals is detected.
To make an accurate diagnosis, laboratory tests are prescribed:
- Urine analysis;
- urine culture with an AB susceptibility test;
- general blood test;
- prostate secretion analysis;
- blood chemistry;
- colon examination.
Additional diagnostics include instrumental research methods. First of all, ultrasound is performed, if necessary, additional MRI and TRUS are prescribed. Relatively recently, a new method of PET examination has emerged, it is considered as more informative.
Treatment of inflammation
Urologists treat all types of prostatitis. Traditional methods are good, but only along with medical prescriptions and with the permission of the attending physician.
First you need to find out the cause of the disease, and only then can you carry out post-symptomatic treatment.
- Active antibiotic therapy helps cure prostatitis. Parenteral antibiotics are most effective.
- With a pronounced pain syndrome, pain relievers and diuretics are indicated.
- For constipation, laxatives are prescribed.
- With severe pain and difficulty urinating, novocaine blockade is established.
- The course of therapy with vitamins and immunocorrectors is indicated.
- It is worth observing a special diet that excludes spicy, salty, smoked dishes.
- Bed rest is prescribed.
From local procedures, sitz baths with water are shown, the temperature of which is two degrees higher than the body temperature. Enemas are made with herbal decoction of anti-inflammatory herbs with the addition of 1% anesthetic, while the contents are slowly injected into the intestine and left there as long as the patient can stand.
Physiotherapy treatment also has a beneficial effect in restoring prostate function. Prostate massage with acute prostate is prohibited, but in chronic form it is recommended. To restore metabolism, normal blood circulation and relief of edema, UHF and microwave are prescribed.
With prolonged urinary retention, a catheter is inserted. At some stages of disease development, surgical treatment is indicated to open the purulent sacs with the installation of drainage.
Treatment of acute prostatitis lasts from a few weeks to a month. A favorable result is usually observed. If the disease has become more complicated or has passed into a chronic stage, the process will be difficult, lengthy and can take several months.
During treatment, restriction of sexual activity and use of personal protective equipment is indicated.
A medical physiotherapy apparatus helps cure prostatitis. Effectively eliminates the symptoms of prostatitis, is able to restore reduced sexual activity, relieve pain, relieve swelling and inflammation. The device can be used at home both for the treatment and prevention of diseases of the pelvic organs.
The device will relieve muscle tension, improve sperm production, strengthen blood vessels and prevent the development of other possible diseases in the pelvis. The device, which treats prostatitis in men, is easy to use, equipped with a regulator of heating and vibration modes and is powered by a network. The compact size allows the device to be used in any condition.
How to prevent the development of the disease?
Preventing different types of prostatitis, like any other disease, is a healthy lifestyle, without bad habits and a balanced diet. If you are diagnosed with prostate, exercises should not be neglected. For any nidus of inflammation that has arisen, you should immediately consult a doctor in order to eliminate the cause and prevent the infection from entering other organs.
You need to make a decent lifestyle, have sex regularly with a regular partner. It is important not to forget personal hygiene of the genitals and not to neglect regular preventive examinations by a urologist. If a man knows what prostatitis can be, and at the same time leads a passive lifestyle, exercises should be done to prevent the appearance of congestion in the small pelvis.
Let us summarize
Depending on the causes and characteristics of the course, acute and chronic types of prostatitis are diagnosed. Chronic pelvic pain syndrome belongs to a special group. Acute prostatitis is characterized by clinical manifestations such as chills, fever, and pain. The chronic form can not appear in any way or has a mild appearance: a violation of urination, painful pain in the pelvic area, which, as complications develop, can lead to impotence and loss of fertility.
Acute prostatitis develops suddenly and is easily diagnosed. In contrast, chronic prostatitis develops in waves, alternating periods of remission and deterioration. In a chronic course, identifying pathogenic microbes can cause certain difficulties. The foci of infection that arise in the genitourinary system provoke complications in the form of diseases of organs that anatomically attach to the prostate gland. Depending on the diagnosed prostatitis, the urologist prescribes a differentiated treatment regimen.






























